WASHINGTON, July 26, 207 - With rural hospitals at risk of closure and healthcare providers increasingly abandoning sparsely populated areas, residents in vast swaths of the country often must drive for hours and take time off from work to see a doctor or medical specialist.
A promising alternative is telehealth, or telemedicine, defined as providing clinical care remotely by two-way video. The practice has been around for decades, but it is still not widely used to provide healthcare services because of restrictions on federal reimbursement, the widely cited problem of inadequate internet connectivity, and the sometimes prohibitive cost of the technology itself, witnesses who support expanded use of telehealth told a House subcommittee July 20.
Nicole Clowers, the Government Accountability Office’s (GAO’s) managing director for health care, told the House Small Business Subcommittee on Agriculture, Energy and Trade and Health and Technology that data from 2014 show that Medicare providers used telehealth services sparingly. “About 68,000 Medicare beneficiaries, or 0.2 percent of Medicare Part B fee-for-service beneficiaries, accessed services using telehealth,” she said, citing an analysis of Medicare claims data by the Medicare Payment Advisory Commission. (The Centers for Medicare & Medicaid Services (CMS), she said, does not limit telehealth and remote patient monitoring use in Medicaid.)
MedPAC also found that 10 states accounted for 42 percent of all Medicare telehealth visits, with South Dakota, Iowa and North Dakota topping the list.
Recent studies have shown rural residents are particularly vulnerable to lack of access to health care. Data from the National Center for Health Statistics show that, adjusting for age, rural whites have 102 more deaths per 100,000 members of the population than their urban counterparts. For rural blacks, the number is higher: They have 115 more deaths per 100,000 than blacks in urban areas.
 But rural areas are underserved, said subcommittee Chairman Rod Blum, R-Iowa. “While 20 percent of Americans live in rural areas, only 9 percent of physicians practice there,” he said. “Telehealth may allow rural physicians to expand their patient base and to keep dollars in the community, benefiting other local small businesses such as retail establishments and restaurants, contributing to the sense of ‘community’ that American small towns pride themselves on.”
But rural areas are underserved, said subcommittee Chairman Rod Blum, R-Iowa. “While 20 percent of Americans live in rural areas, only 9 percent of physicians practice there,” he said. “Telehealth may allow rural physicians to expand their patient base and to keep dollars in the community, benefiting other local small businesses such as retail establishments and restaurants, contributing to the sense of ‘community’ that American small towns pride themselves on.”
Barb Johnston, CEO of HealthLinkNow in Sacramento, California, echoed Blum, stating that telemedicine benefits not just individual residents but their communities as well. She cited research done on 24 rural communities in Kansas, Oklahoma, Texas and Arkansas that showed significant cost savings on health care personnel and transportation, as well as reduced pharmacy/lab costs. In addition, people did not have to miss work to visit a doctor or hospital.
But there are barriers to providing telehealth services, Johnston and other witnesses said. She suggested that the Drug Enforcement Administration modify its rules to allow physicians to prescribe controlled substances by telemedicine. This would benefit opiate addicts who need medication-assisted treatment; veterans with post-traumatic stress disorder and traumatic brain injury; and children with attention deficit hyperactivity disorder.
She also recommended a change to CMS regulations in order to allow Medicare patients to receive telehealth services no matter where they live. Currently, Medicare will only reimburse telehealth services provided outside a Metropolitan Statistical Area (defined as having a core urban area of 50,000 or more people) and patients must live in or receive services in a federally designated Health Professional Shortage Area.
“Medicare treats telehealth almost exclusively as a tool for rural areas, and has narrowly restricted the geographic areas that are eligible to use telehealth,” according to the Center for Connected Health Policy. Johnston noted that “Medicare is the only health insurance payor who limits access to healthcare via (telemedicine) related to geography” and added, “If that one thing could get corrected, I think the market would drive expansion” of telemedicine services.
At the hearing, she also said Medicare’s rural restriction has led many health facilities to refuse to provide telehealth services because of concerns over billing problems – specifically, that they will be perceived as providing preferential treatment to non-Medicare patients.
Patients also cannot be at home: According to Clowers’ testimony, “Medicare requires that the patient be physically present at a medical facility such as a hospital, rural health clinic, or skilled nursing facility.”
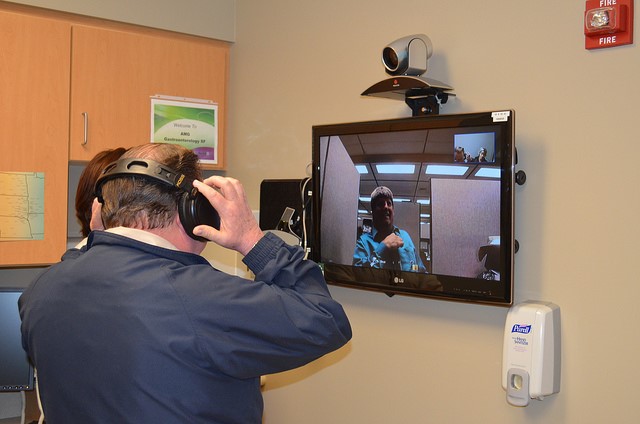
A USDA official tests out the telemedicine equipment during a tour of Avera Health in Sioux Falls, South Dakota
Johnston recommended simplifying “national credentialing and state reciprocal medical licensing processes to enable telemedicine psychiatric and specialist medical services to be increasingly linked into rural primary care clinics,” which would “give rural communities better access to medical experts.”
An example of the benefits of telehealth was provided by Michael Adcock, executive director of the Center for Telehealth at the University of Mississippi Medical Center (UMMC). Mississippi leads the nation in its rates of heart disease, obesity, cardiovascular disease and diabetes, but Adcock noted that treating these conditions “is made harder by the rural nature of our state” and that more than “traditional, clinic and hospital-based services” are needed.
Adcock described a pilot program to use remote patient monitoring to help diabetics in the Mississippi Delta. “The program allowed doctors and other health practitioners to treat patients remotely, in real time and at home, using online streaming video technology and other tools for two-way live communication,” according to UMMC.
After six months, preliminary results showed “a marked decrease in blood glucose, early recognition of diabetes-related eye disease, reduced travel to see specialists and no diabetes-related hospitalizations or emergency room visits among our patients,” Adcock told the subcommittees.
“Teaching them to take care of themselves was the biggest success factor,” Adcock said.
“This pilot demonstrated a savings of over $300,000 in the first 100 patients over six months,” Adcock said. “The Mississippi Division of Medicaid extrapolated this data to show potential savings of over $180 million per year if 20 percent of the diabetics on Mississippi Medicaid participated in this program.”
Businesses also have the option to participate in UMMC’s telehealth program, Adcock said, seeing it as a way to support their employees and reduce costs incurred for after-hour clinic visits and emergency room visits for non-emergency conditions.
Although the hearing focused primarily on telehealth, David Schmitz, president of the National Rural Health Association, also emphasized the importance of programs to incentivize the training of doctors in rural areas and preventing the closure of rural hospitals, 81 of which have shut their doors since 2010.
“Because hospitals provide so many jobs, it follows that their closure has a devastating effect on employment,” Schmitz said. “If Congress allows the 673 additional vulnerable rural hospitals to shut their doors, 99,000 direct health care jobs and another 137,000 community jobs will vanish.”
#30


